One of the key issues undermining health in the United States and especially here in Tampa, Fla., is the simple fact that our modern healthcare system treats patients as consumers instead of as partners in health.
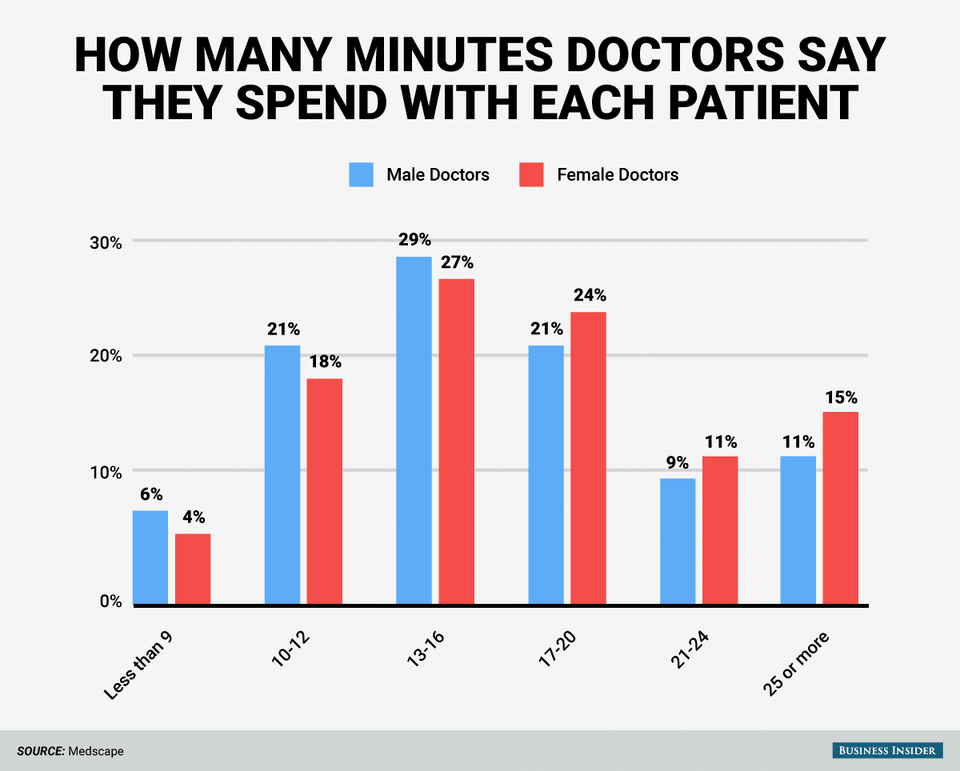
The average primary care physician sees three to four patients per hour. That averages out to about 15 to 20 minutes per patient visit, not counting the time the doctor spends between patients and time spent writing prescriptions, ordering and reviewing test results, and so on.
Subtract that time, and we estimate the average time a doctor actually spends communicating with a patient is about seven minutes.
Seven minutes is certainly enough time for a doctor to hear a patient describe one or two primary symptoms and to write a prescription or make a referral to a specialist.
However, it is not nearly enough time for a doctor to establish the sort of partnership with a patient that enables the doctor and patient to work as a team to restore optimum health.
Seven minutes is not even enough time to sort through the long list of possible physical, emotional, environmental, and lifestyle factors that could be contributing to a patient’s illness and work with the patient to address these potential underlying causes.
Doctors don’t limit their time with patients by choice. Most doctors would like to spend more time with each patient, but they’re restricted from doing so by insurance companies or the practice in which they work.
Compensation for most general practitioners has tied not to effective treatment outcomes or patient satisfaction but to the number of patients they see. As a result, doctors who spend less time with patients generally:
- Write more prescriptions
- More frequently refer patients to specialists
- Are at a greater risk of malpractice claims
Quick Fix Medicine — it’s a Costly Solution
Despite some of the miracles of modern medicine and the growing interest in Functional Medicine in Tampa (which is what we practice at BioDesign Wellness), the current healthcare system is a disaster.
Although we are often told that the U.S. healthcare system is the best in the world, it actually ranks last of in the list of the 11 highest-income countries.
According to the Commonwealth Fund, the U.S. “leads the world in health care spending, but residents are sicker and more likely to die of preventable conditions than those in other wealthy countries.”
Specifically, according to the Commonwealth Fund’s Eric C. Schneider, M.D. (the organization’s senior vice president for policy and research) and David Squires (the fund’s former senior researcher), the U.S. healthcare system faces four primary challenges:
- High costs
- Difficulty accessing primary care
- Confusing and inefficient administration
- Disparities in care because of income, education, level, race, or ethnicity
Although we agree that the U.S. healthcare system is challenged, we disagree with the causes. The real issues that are causing healthcare costs to soar while people become sicker in the U.S. (and in many other developed countries) are these:
- Compensation and profits in the medical industry are tied not to positive patient outcomes but to the number of patients seen, number of medications prescribed, and the number of surgeries and other medical procedures provided
- The conventional medical system focuses more on identifying and alleviating symptoms than on restoring health
- Uneducated, disengaged patients do not play an active role in achieving and maintaining optimum health
- Poor nutrition due to unhealthy dietary choices and a food supply that is dwindling in nutritional value
- Increasing exposure to higher levels of toxins in the products we buy; the buildings in which we live, work, and study; the foods and other products we consume; and even in the natural environment
- An increasingly sedentary culture/lifestyle
- Overmedication, wrong medication, unnecessary surgeries, and other medical interventions that impair the body’s healthy function
When the Cure Is Worse Than the Illness
During the seven minutes or so that a conventional doctor spends with a patient, the doctor is under intense pressure to diagnose and treat.
The rush from diagnosis to treatment often results in a quick fix that does nothing to restore the patient’s health and, even worse, actually causes or contributes to other long-term illnesses.
This is hardly in keeping with Hippocrates’ age-old admonishment: “First, do no harm.” Here are a few cases in point:
-
The opioid epidemic: The current opioid epidemic is a symptom of a very sick healthcare system. Instead of treating the underlying cause of pain, which is often inflammation, many doctors chose the quick fix — writing prescriptions for powerful painkillers.
According to the National Institutes of Health, the number of deaths involving opioids in 2017 alone was 49,068. Deaths related exclusively to opioid pain relievers (in 2016) were 19,354!
-
Acid reflux: According to the American College of Gastroenterology, many people who take popular antacid pills such as Nexium, Prevacid, and Prilosec don’t need them, and these proton pump inhibitors (PPIs) are known to be overprescribed. The trouble is the body needs stomach acid to digest food fully and to keep certain infections at bay.
For example, published studies have linked PPIs to an increased risk of potentially deadly diarrhea caused by the bacteria Clostridium difficile (C. diff.), which makes patients more prone to pneumonia.
PPIs have also been linked to inhibiting the body’s absorption of calcium and magnesium, which leads to an increased risk of bone fractures, especially in women.
-
Low cholesterol: Doctors continue to focus on high levels of low-density cholesterol (LDL) as a primary culprit in heart disease, and they continue to prescribe statins to lower LDL when the real culprits are abnormal blood cholesterol and belly fat caused by overconsumption of sugar in all its forms, including flour and refined carbohydrates.
Not only do statins target the wrong cause of cardiovascular disease, but they can contribute to a host of additional health problems, including muscle pain, muscle damage, memory issues, and Parkinson’s-like symptoms. They also increase the risk of diabetes by about 50 percent.
-
Autoimmunity: Autoimmune disorders occur when the immune system attacks healthy cells in the body by mistake, which often causes inflammation. Conventional medicine often relies on medication to reduce inflammation.
However, treating the inflammation with prednisone, steroids, antihistamines, and other medications ignores the underlying triggers and often leaves patients with additional symptoms or side effects and an ongoing and sometimes increasing need of medications.
Patients with autoimmune issues have very complex issues that take time to identify and resolve. Identifying and eliminating or avoiding triggers, adjusting diet and lifestyle, and using holistic therapies are effective in managing autoimmune disorders.
Proper diagnosis and treatment are impossible in the span of a 7-minute doctor visit. The right approach requires several hours with a doctor over a period of twelve months to monitor progress and adjust treatments as the patient’s health is restored.
-
Chronic inflammatory response syndrome (CIRS): Often caused by exposure to toxic mold and other environmental toxins, chronic inflammation affects a number of the body’s systems (muscular, skeletal, respiratory, circulatory, digestive, and so on).
For one patient, it manifests as itchy skin, brain fog, and sinusitis. Another patient may have fatigue, joint pain, leg cramps, and memory loss. Many patients have more than a dozen symptoms impacting different systems.
Again, practitioners of conventional medicine often treat the symptoms without addressing the underlying causes. As a result, patients may suffer for their entire lives without an accurate diagnosis or effective treatment.
-
Chronic infections: Sinusitis, ear infections, pulmonary infections, gastrointestinal (GI) infections, urinary tract infections, and other chronic or recurring infections are often treated with repeated courses of antibiotics, which are not only ineffective long-term solutions but also cause additional problems.
First, they kill healthy gut bacteria, thus weakening the body’s immune system. Second, when they fail to kill all the harmful bacteria, the surviving bacteria are more resistant to antibiotics.
In fact, overuse and misuse of antibiotics have led to the creation of superbugs, which modern medicine is finding very difficult to treat.
The problem in all of these examples is that many doctors skip essential diagnostic steps in an attempt to take a shortcut to treatment. They don’t ask important questions, such as, “Why does this person have these symptoms?” Instead, they label and treat:
- When blood pressure is high, they prescribe medication to lower it.
- When a patient reports indigestion, they label it acid reflux and prescribe medication to reduce stomach acid.
- When thyroid hormone is low, they prescribe synthetic thyroid to raise levels.
As you can see, conventional doctors stop at the label when they should be asking questions such as “Why is this person’s blood pressure high?” “Why is this patient having indigestion?” and “Why is this person’s thyroid hormone low?”
Diagnosis without attention to a cause is limiting, and too often, this is the approach in the current healthcare system. Unfortunately, the system doesn’t encourage doctors to dig deeper to identify and address underlying causes.
The right approach isn’t possible with two to three 7-minute office visits over the course of the year. The right approach requires a careful and detailed investigation into the cause(s) — medical history, family history, diet, lifestyle, emotional stress at work or home, exposure to environmental toxins, and so forth.
In addition, effective treatment involves more than popping a pill or having a one-time surgery or other medical procedure.
It requires patient involvement and effort, which often necessitates that the doctor or someone in their practice serves as a health coach of sorts — educating the patient on what’s causing the illness and what adjustments the patient needs to make and then encouraging the patient and holding him or her accountable for making the necessary adjustments.
None of this is possible in the course of a short series of 7-minute office visits.
Why We Tolerate a Broken Healthcare System
The current healthcare system is broken, so why don’t we fix it? Here are some of the reasons:
- The healthcare industry is booming. From a financial standpoint, the industry is not broken; it’s thriving. Hospitals, pharmaceutical companies, and other providers and suppliers have little incentive to fix a system that’s generating so much profit.
- Many people have insurance to cover a good chunk of the costs, so they take what they can get. In addition, when insurance companies choose not to cover the cost of “alternative” healthcare, people have a disincentive to seek long-term solutions, such as those provided by functional medicine practitioners.
- People are known to be lazy. We want a quick fix. We don’t want to spend the time and effort to eat healthy, exercise, and relinquish the dream of “better living through chemicals” (such as dry cleaning, household cleaners, manufactured pesticides, plastics, and so forth).
- We’re hedonists at heart. Unless we make a conscious effort to control our cravings, we tend to overindulge in processed carbohydrates, alcohol, nicotine, and other unhealthy delights. And rarely do we ever dig deep to determine why we reward ourselves with food instead of a run, walk, or game of tennis.
- We are reluctant to rock the boat. When people fight against conventional medicine, they pay the price for it. Just look at what happens to doctors and parents who try to initiate more reasonable vaccination protocols.
Weighing the Costs
Many people who recognize the benefits of integrative healthcare feel discouraged by the costs and lack of insurance coverage for alternative diagnoses and treatments.
They may be able to see a conventional doctor for free or for a low copay of $20 or so, whereas a visit to a functional medicine practice is likely to cost hundreds of dollars.
However, you would be wise to reconsider the costs:
- Most general practitioners charge over $150 per visit, which covers about 15 minutes of their time. If a functional medical practice charges $300 or $400 for a one-hour visit, consider it a bargain.
- Paying more for an accurate and complete diagnosis and more effective long-term treatment makes sense. What does not make sense financially or physically is paying for treatment that fails to restore health and has a higher chance of contributing to other health issues in the future.
- Expect to pay more in time and effort with a functional medicine doctor. This is not a relationship in which you passively receive care. You play an active and integral role in diagnosis and treatment. Achieving and maintaining good health takes time and effort, but the investment pays huge dividends.
What Makes BioDesign Wellness Center Better?
At BioDesign Wellness Center, we provide the care you need outside of the current healthcare system while using your insurance for labs. This gives us the time we need to solve the medical mysteries underlying whatever symptoms we are experiencing.
We do not substitute for your current internist or specialist; instead, we become a part of your diagnostic and treatment team. Our job is to fill in the blanks that are impossible to cover over the course of only a few 15- to 20-minute visits with your conventional docs.
This approach enables your entire treatment team to provide the integrative care you need as affordably as possible.
At BioDesign, we begin building the doctor-patient relationship through education prior to your first visit. During your free new-patient orientation session, you spend an hour with one of our doctors, nutritionists, or patient educators, who brings you up to speed on our treatment approach and what makes it so unique.
Included is a discussion of the current healthcare system, the role stress plays in your life, the role of hormones in achieving optimal health, the importance of proper nutrition, and patient examples that reveal what you can expect.
We also have a specific presentation for prospective patients who want to find out whether living or working in a water-damaged building (WDB) is causing them to be ill.
Patients who attend the initial workshops will have a reduced visit fee if they decide to move forward with a consultation. We can offer this discount because the orientation session makes you a more educated and proactive patient, which saves us time and effort moving forward.
We strongly recommend that you bring your spouse or significant other to the patient orientation because your health is often interdependent, and the information shared will increase participation and support in your care.
The importance of engaging your spouse or significant other in the process cannot be overstated. If you had cancer or a heart attack, your spouse would attend doctors’ visits and education sessions with you.
At BioDesign Wellness, we just might be the deciding factor in helping you or your loved ones become future cancer or heart disease patients.
If you have already been there, we will work with you to be proactive and reduce the modifiable risks associated with a reoccurrence in ways that many in the current healthcare system are ignoring due to a lack of time or information.
After completing one of our programs, your optimal health will start to come into sight, and you will have identified one or more sources for why you have been suffering, allowing you to move forward in a proactive manner that is truly life-changing. See the difference for yourself.
The only way you will know is to step out of the current healthcare system and step into something more practical and personalized.
To schedule a new patient orientation (there is no initial fee), contact our Patient Care Coordinator, Lori, to reserve your time. Patient orientation sessions are usually conducted twice a month, and sessions fill up quickly. Lori can be reached by calling (813) 445-7770.
———
Disclaimer: The information in this blog post about the length and scope of an appointment with a traditional doctor is provided for general informational purposes only and may not reflect current medical thinking or practices. No information contained in this post should be construed as medical advice from the medical staff at BioDesign Wellness Center, Inc., nor is this post intended to be a substitute for medical counsel on any subject matter. No reader of this post should act or refrain from acting on the basis of any information included in, or accessible through, this post without seeking the appropriate medical advice on the particular facts and circumstances at issue from a licensed medical professional in the recipient’s state, country or other appropriate licensing jurisdiction.